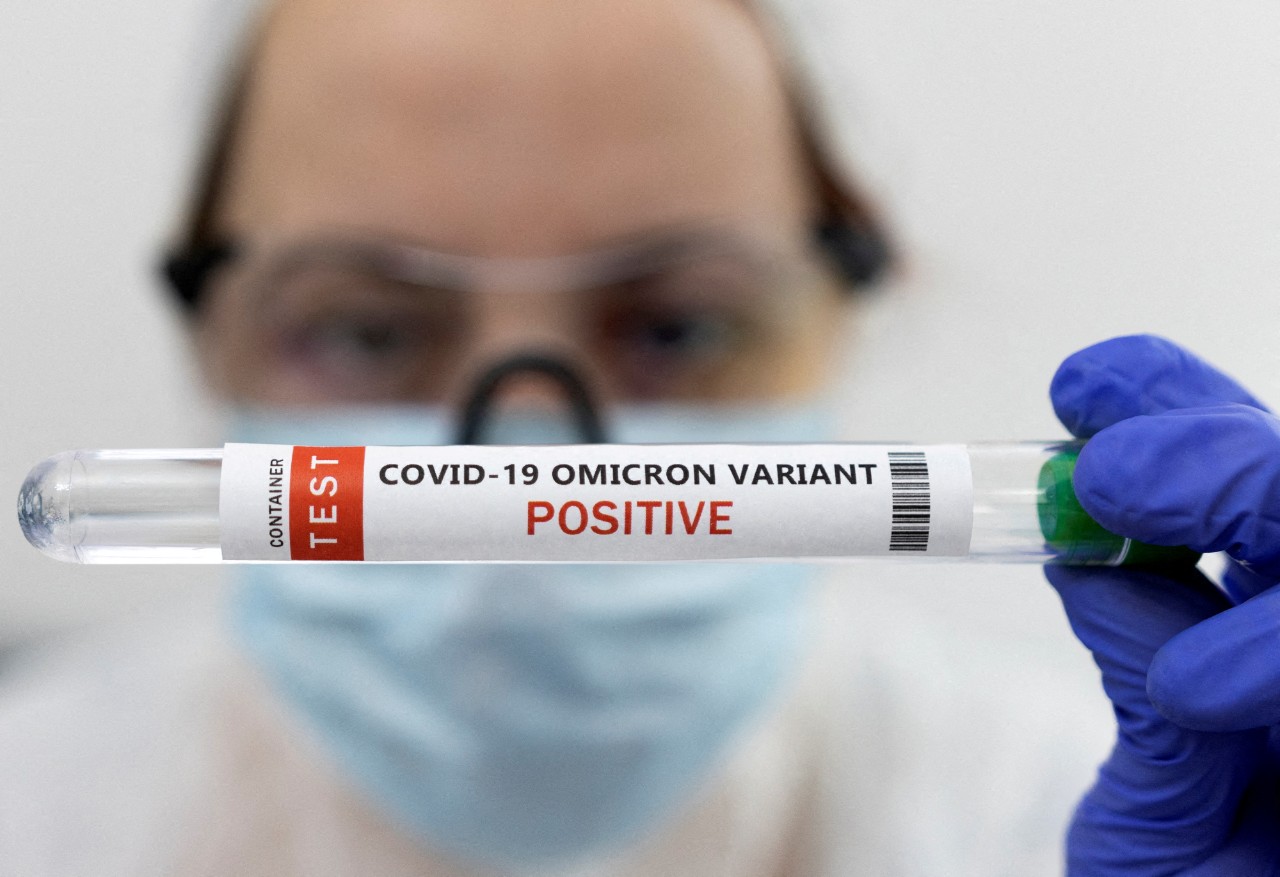
Omicron’s high transmissibility, coupled with vastly different rates of vaccination worldwide and a wide range of varying strategies have made the pandemic’s future difficult for experts to model.
As the coronavirus pandemic took hold in 2020, health officials held out hope for vaccines to assist in providing the so-called herd immunity, the state that exists when so many people have either been vaccinated or have contracted and recovered from a disease that it becomes endemic, and not a major threat to the health of a population.
In 2021, the vaccines offered great hope – and here in Malaysia, the rollout was a laudable success – but Omicron shifted the narrative again, as the variant demonstrated that, even though its symptoms were milder, it had developed a better ability to evade immunity, whether that immunity had been induced by vaccination or by prior infection.
Still, some experts believed – or perhaps hoped – that given Omicron’s extremely high transmissibility and milder symptoms, herd immunity was still a vaccine-led possibility, though perhaps just more of a moving target.
A growing body of evidence, however, is now challenging that hope.
OMICRON WAS A GAME-CHANGER
Soon after Omicron was discovered and identified, researchers foresaw problems. The variant had far more mutations, including a lot more on the spike protein (the part of the virus that directly interacts with our cells), making it likely that the mutated virus would be better able to evade our immune protection. That has proven to be the case, and the only saving grace has been that the symptoms from this variant are relatively milder than those of previous strains, particularly the widespread Delta variant. (It is largely accepted that this is due to the virus generally confining itself to the upper respiratory tract of its host, resulting in less severe symptoms.)
Though some experts still hold that the combination of being fully vaccinated and boosted AND having contracted and recovered from a Covid infection, even Omicron, induces a gold standard of individual immunity, the notion that this will lead to herd immunity may be getting challenged by the sheer speed at which Omicron spreads.
Cases of Omicron infections can double in less than two days, which is much faster than previous coronavirus variants and closer to what public health experts would expect from the milder influenza virus. “Omicron is flu [influenza] on acid,” one scientist explained.
The breakneck speed of Omicron’s spread has meant, in many cases, that vaccines simply cannot keep up, as there is a latency period between the time of the jab and the time the vaccine’s maximum efficacy is reached.
“We hadn’t seen that speed before, and it meant you couldn’t vax your way out of it,” said Christina Pagel, a healthcare data analyst at University College London. “Even if you could vax everybody, it still takes two weeks for the vaccine to kick in, and by then you’re in the middle of it.”
That reality has put government officials and the health experts who advise them in a very difficult position. “It was a situation where you either put in restrictions very, very early, or you do nothing,” Pagel said. “But if you wait to see what happens, then it’s too late.”
The UK got a taste of this firsthand after enacting restrictions in December following reports of the Omicron variant’s discovery and identification in South Africa. By the time the new measures were put into place, however, it was too late: Omicron was not only already present in the UK, it was spreading like wildfire.

UNKNOWN… AND PERHAPS UNKNOWABLE
In the early months of the pandemic, experts could model their analyses on the assumption that most people worldwide were equally at risk of infection, because Covid-19 was a novel, new disease and, at that time, no vaccines were available.
But by late in 2021, following nearly a full year of not only having different vaccines, but also of different vaccine strategies, along with variable rates of vaccination from country to country and differing rates of infection and recovery, the immunological landscape – and the ability to accurately forecast the ‘track’ of the pandemic – had changed dramatically, to the point where some experts began conceding that it’s just not possible to predict how the coming months are going to play out.
Some, however, believe that the notion of true herd immunity may be slipping out of reach.

“Reaching a theoretical threshold beyond which transmission will cease is probably unrealistic, given the experience we have had in the pandemic,” Dr Olivier le Polain, an epidemiologist with the World Health Organization (WHO), remarked recently in an interview with Reuters.
That said, it doesn’t mean that previous immunity confers no benefits at all – far from it. Instead of the much-touted herd immunity, health experts have noted that there is growing evidence that vaccines and prior infection would simply continue to help boost population immunity against Covid-19, which makes the disease less serious for those who are infected, or become reinfected. And that’s certainly not nothing, nor does it mean the vaccines aren’t doing their job. Growing immunity within a population is always a good thing which it comes to epidemics or pandemics. It’s just that the threshold at which we can realistically achieve real herd immunity has proven to be a consistently shifting goalpost, and we’re unlikely to hit the vaccine penetration needed, and certainly won’t do so by the time the next mutation arrives on the scene. But that doesn’t mean all hope is lost.
“As long as population immunity holds with this variant and future variants, we’ll be fortunate and the disease will be manageable,” explained Dr David Heymann, a professor of infectious disease epidemiology at the London School of Hygiene and Tropical Medicine.
A VICTIM OF THEIR OWN SUCCESS?
Any vaccine is generally meant to stave off the worst outcomes of a disease. Every now and then, however, a vaccine can be so effective, it helps bring about the end of a disease – or close to it. Take measles, for example, an incredibly virulent and highly contagious disease that was curbed by vaccines.
As the Covid vaccines began coming to market, the efficacy rates of some of them proved to be remarkably high, surpassing all expectations.
Owing partly to our collective, desperate desire to exit the pandemic and partly to some legitimately mixed messaging, people began – incorrectly – to view the vaccines as an impenetrable shield against any infection, rather than as just one more weapon in the arsenal against Covid.
So, unsurprisingly, when breakthrough cases occurred, and vaccinated people contracted the virus, anti-vax critics were quick to pounce, pointing to this as a failure. But it wasn’t; the Covid vaccines overwhelmingly still keep people out of the hospital and out of body bags, which is their function.
And so still, with rates of effectiveness against hospitalisation and death of over 80%, and even 90% for a number of the vaccines, people have still held out hope that widespread inoculations will bring Covid-19 under control and possibly even spell the end of the pandemic.

But three things have muted those hopes, if only slightly. First, vaccination rates worldwide are woefully uneven. Many countries and regions have not even achieved 25% vaccine coverage, as wealthy countries are getting vaccinated at more than 10 times the rate of poorer countries.
Second, it’s been shown that the protection given by these vaccines wanes relatively quickly – often in a matter of months. Booster shots have helped push that efficacy back up, and significantly so, but it’s as yet unknown if that round of jabs will offer a longer-lasting immunity.
(It’s important to note here, however, that the effective protection afforded by the vaccines doesn’t evaporate completely over time, it just decreases. Dropping from 93% effectiveness to 65% effectiveness, hypothetically speaking, might look really bad on paper, but a lot of vaccine efforts would be doing well to get to 65% in the first place. The Covid vaccines were just so monumentally effective from the get-go that we’ve set the bar higher than normal. Additionally, for vaccinated individuals who contract the Omicron variant’s infection, recovering from that infection still enhances immunity, as well.)
The third, finally, is simply down to the nature of viruses. They evolve and mutate in order to ‘survive’ and to continue carrying out their mission, which is to replicate as many times as possible, infecting as many hosts as is necessary to do so. That, experts have noted, is one likely reason Omicron is so contagious yet much less deadly.
“A virus that’s so lethal that it kills its host, especially quickly, is a failure as a virus,” one researcher said. “Once the host dies, the virus can no longer replicate. The successful virus will infect, but not kill, its host, so that it can continue replicating and spreading.”

HERD IMMUNITY THE HARD WAY
The SARS-CoV-2 coronavirus has so far been a master of survival, having mutated rapidly and repeatedly, spawning a number of variants in 2021 alone. That’s made it challenging for vaccines to keep up, and Omicron has proven to be the most successful yet at evading immunity. Worse still, that ability enables Omicron to dodge one person’s immunity and use that loophole to spread to others, oftentimes asymptomatically and undetected.
“It changes the game when vaccinated people can still shed virus and infect other people,” said Dr David Wohl, an infectious disease specialist at the University of North Carolina’s School of Medicine.
Wohl also noted that just contracting and recovering from an Omicron Covid infection is no guarantee you won’t get infected by it again – or by the next variant that comes along. “Just because you had Omicron, maybe that protects you from getting Omicron again… maybe.”
Other experts have been even less sanguine in their assessments. The WHO’s Dr le Polain said that he still expects Covid-19 to become endemic, to a point where it will continue circulating in the population and cause occasional surges here and there, but explained that the rise of the Omicron variant threw into doubt exactly when that might happen. “We will get there,” he said, “but we are not there at the moment.”
Francois Balloux, professor of computational systems biology at University College London, noted in a recent interview that lofty expectations had been set early on, perhaps unrealistically, saying, “These things were in the media: ‘We’ll reach herd immunity when 60% of the population are vaccinated.’ It didn’t happen. Then for 80%. Again, it didn’t happen.”
He added, “As horrible as it sounds, I think we have to prepare ourselves for the fact that the vast majority, essentially everyone, will get exposed to SARS-CoV-2.”
Reports from Reuters, Quartz, the World Health Organization, Nature.com, Bloomberg, and News-Medical.net contributed to this article.
"ExpatGo welcomes and encourages comments, input, and divergent opinions. However, we kindly request that you use suitable language in your comments, and refrain from any sort of personal attack, hate speech, or disparaging rhetoric. Comments not in line with this are subject to removal from the site. "