It’s accepted science that people with certain blood types have a lower risk for a number of various illnesses. Some studies suggest Covid-19 might be one of them, but a conclusive answer is much less clear.
Do you know your blood type? Depending on what it is, you might have an increased risk or a reduced risk for certain illnesses or health conditions.
You can’t tell by looking at a person, but each of us has a defined blood type running through our veins. Many people never find out their type until it becomes necessary for one reason or another, and in reality, your blood type doesn’t really matter that much – that is, until it does.
Need a blood transfusion? Are you donating blood? Going through pregnancy? Then you’ll likely find out in a hurry why your blood type actually is a matter of well-hidden importance.
WHAT DOES BLOOD TYPE MEAN, ANYWAY?
Here’s a quick refresher for those who may have long forgotten those anatomy and physiology courses taken long ago.
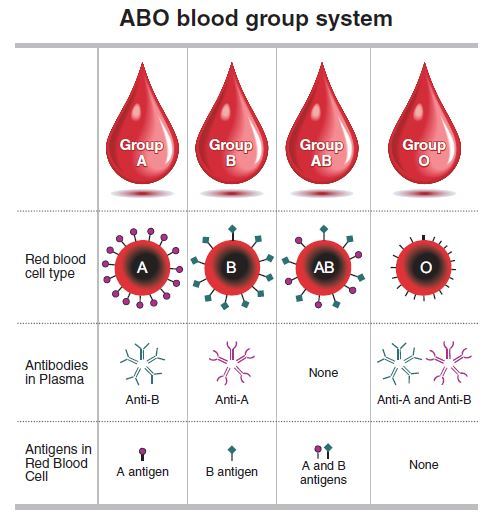
The letters A, B, and O represent different variants of the ABO gene, which is what programs our blood cells to form the different blood groups. If you have type A blood, your body is programmed to produce the A-type antigens on red blood cells. Type AB blood, on the other hand, would result in both A and B antigens being produced on red blood cells. A person with type O blood doesn’t produce any antigens. (Antigens are substances which induce an immune response, particularly in the production of antibodies.)
On that point, type O blood carries both anti-A and anti-B antibodies in the plasma. Type A carries anti-B antibodies only; type B carries anti-A antibodies only; type AB carries no antibodies.
Along with the letter code for blood types, there’s also a Rhesus factor, or “Rh,” which is an inherited trait. A blood type is said to be “positive” or “negative” depending on whether there are proteins on the red blood cells or not. If your blood has proteins, you’re Rh-positive. If not, you’re Rh-negative.
Given the four main blood groups (A, B, AB, and O) and two Rh factors for each (positive or negative), there are a total of eight blood types.
These factors all come into play most commonly when donating or receiving blood. People with type O- (O negative) blood are considered universal donors, because their blood cells don’t have any antigens or proteins, meaning anyone’s body will be able to accept it in an emergency. Think of that blood cell like an empty thumb drive that any computer can accept and write its own programs on.
Conversely, sticking with this analogy, someone with type AB+ has a thumb drive that’s already full and coded, and thus can’t easily be used by just any computer. Biologically, their blood cells are already carrying antigens and proteins of their own, and would be rejected by others’ bodies unless the “program” was the same.
Additionally, type O blood carries both anti-A and anti-B antibodies in the plasma. Type A carries anti-B antibodies only; type B carries anti-A antibodies only; type AB carries no antibodies.
HOW DOES BLOOD TYPE RELATE TO COVID?
Medical experts know that a person with type A, B, or AB blood will be a bit more likely to develop heart problems, experience heart failure, or suffer a heart attack. People with types A or B blood are also more susceptible to problems like deep vein thrombosis, pulmonary embolisms, or blood clotting disorders.
Covid-19, in serious cases, can cause heart problems, blood clotting, and other cardiovascular issues. So could there be a connection between blood type and the severity of illness cause by Covid?
Some doctors believe that the growing body of anecdotal cases which suggest a link, such as a decreased risk of severe illness from Covid-19 in people with type O blood, is part of this same body of evidence. Research is ongoing, but as of now, the findings are still inconsistent and inconclusive.
As reported by CNN in the first year of the pandemic, a team of European researchers who published their findings in the New England Journal of Medicine in June 2020 found people with type A blood had a 45% higher risk of becoming infected than people with other blood types, and people with type O blood were just 65% as likely to become infected as people with other blood types. They studied more than 1,900 severely ill coronavirus patients in Spain and Italy, and compared them to 2,300 people who were not sick.
A similar effect for Hong Kong health care workers with blood group O was observed during the SARS outbreak, which infected 8,098 people from November 2002 to July 2003 and is from the same family of viruses.
However, even at that time, there was uncertainty about any significant correlation between blood type and Covid susceptibility. A year later, such a connection was even less clear.
According to one comprehensive paper titled “Relationship between blood type and outcomes following Covid-19 infection,” published in 2021, four out of five studies have shown a lower risk of viral infection, serious illness, and mortality from Covid-19 for people with any Rh-negative blood type.
Similarly, studies also demonstrated a possible correlation between ABO-typing and susceptibility to infection. Overall, eight out of nine studies confirmed this connection.

A majority of the studies showed that type O- blood offered the greatest protection from a multitude of Covid-caused outcomes ranging from infection and hospitalisation to mechanical ventilation and death.
Seems fairly convincing, right? A closer read reveals a major caveat, however. As the paper notes of one study it analysed, “Although the data are convincing, this study was limited by the inability to test critically ill patients who died quickly after hospital admission.”
Most of the other studies had similar limitations, resulting from sample size, missing blood types, and other incomplete data points.
The paper’s conclusion, after analysing the results of many studies, seemed to suggest its authors were hedging their bets, noting, “Although these reports might be inconsistent in their findings, certain trends are evident. Many studies report that blood type A might predispose one to increased susceptibility of infection with SARS-CoV-2, and type O and Rh-negative blood groups might be protective.”
Ultimately, they found an insufficient body of conclusive, consistent data to demonstrate a clear correlation between blood type and Covid-related severe illness or mortality, but noted that anecdotal evidence warranted further study. They also noted that their analysis of the current literature did not warrant using blood type as a predictive tool or as a method of triage for Covid patients.
So, while the research that’s currently available certainly shows that blood type can possibly tip the scale in terms of overall risk of developing heart disease, that doesn’t necessarily translate fully to Covid susceptibility. Additionally, larger factors such as diet, exercise, and environmental pollutants or exposure to hazardous materials are also major players in determining a person’s cardiovascular health.
Information from the Mayo Clinic (mayoclinic.org), WebMD, the US National Library of Medicine, the UK NHS, CNN, and CNET.com contributed to this article. The article is intended for informational purposes only, not as a substitute for advice from a licensed medical professional.
"ExpatGo welcomes and encourages comments, input, and divergent opinions. However, we kindly request that you use suitable language in your comments, and refrain from any sort of personal attack, hate speech, or disparaging rhetoric. Comments not in line with this are subject to removal from the site. "



















